An 80-year-old male presented to hospital with fresh per rectal bleeding and multiple falls. His medical history included iron deficiency anaemia, atrial fibrillation, single chamber permanent pacemaker, chronic kidney disease stage 4, non-ischaemic cardiomyopathy of unclear aetiology and monoclonal gammopathy of undetermined significance (MGUS). Examination revealed periorbital ecchymosis (racoon eyes) (Figure 1) and macroglossia. Urinalysis showed 2+ proteinuria and a raised urinary albumin creatinine ratio (14.17). Renal ultrasound identified normal sized kidneys. Both Kappa and Lambda serum free light chains were identified on previous blood tests. Due to the periorbital ecchymosis and history of falls, CT head and orbit was organised. This ruled out any fracture of the orbital bones but demonstrated bilateral thickening of the extraocular muscles (Figure 2). The patient was too frail to tolerate either cardiac MRI or tissue biopsy. In light of the patient’s progressive condition, underlying comorbidities, advanced frailty and personal wishes, he was commenced on palliative care.
Figure 1 Periorbital ecchymosis (racoon eyes), classically seen in AL amyloidosis
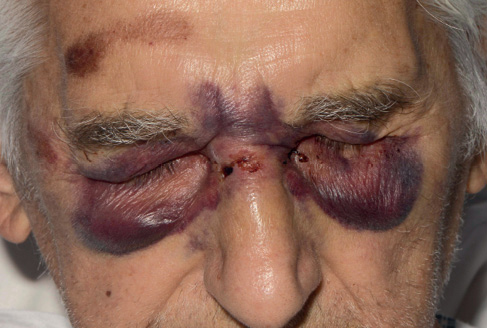
Figure 2 Extraocular muscle thickening on CT imaging (mainly inferior, medial and superior recti)
The combination of periorbital ecchymosis and macroglossia in the context of multiple system involvement is highly suggestive for systemic amyloid light-chain (AL) amyloidosis. The presence of elevated serum free light chains in our patient with normal kidney size on an ultrasound and extraocular muscle thickening on a CT scan are also consistent with this diagnosis. MGUS is the most common plasma cell dyscrasia to affect elderly patients.1 Whilst MGUS itself is an asymptomatic premalignant disorder, it is also a known precursor of more serious plasma cell malignancies such as AL amyloidosis.2 Systemic amyloidosis causing enlargement of the extraocular muscles has rarely been mentioned in literature.3 Interestingly, per rectal bleeding has been reported as a clinical presentation of amyloidosis of the gastrointestinal tract.4 AL amyloidosis is a challenging disease to diagnose due to its insidious presentation and diverse clinical manifestations.5 Correlating clinical signs with laboratory investigations and medical imaging is key to making a diagnosis, particularly in elderly patients where invasive biopsy, and therefore histological diagnosis, is not practical. AL amyloidosis is a progressive, non-curable disease. Life-prolonging treatments such as chemotherapy, stem-cell transplantation and organ transplantation are rarely options for elderly patients, particularly in the context of multiple system progressive disease. Symptom control and consideration of patient wishes should instead be a clinician’s main focus of care. 
