A 38-year-old female with acute lymphoblastic leukaemia on treatment was admitted with new onset diplopia of two days duration. She had recently finished a course of anti-tuberculous treatment for pulmonary tuberculosis. On examination, she afebrile, had a partial ptosis of the right eye, a right fixed and dilated pupil, and impaired downgaze most evident in the primary position and medially suggestive of IR palsy (Figures 1 and 2). Other movements of the right eye were preserved. There were no other focal neurological deficits.
Figure 1 Top panels show a mydriatic pupil on the right side with a normal pupil on the left. Bottom panels show a right downgaze palsy with preserved upgaze
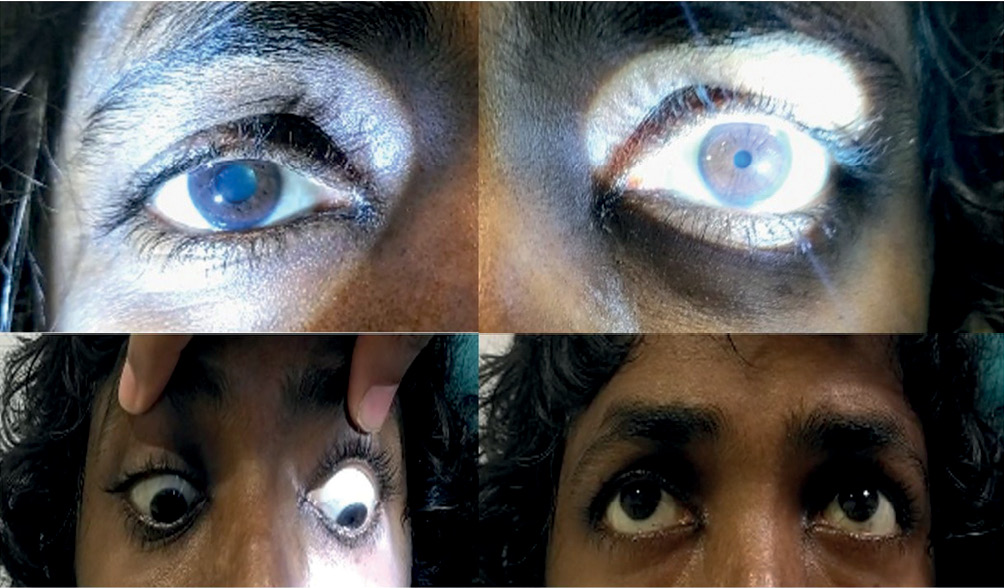
Figure 2 Diffusion weighted magnetic resonance image shows a midbrain lacunar infarct. Diagrammatic representation on the left shows the fascicular arrangement in the medial midbrain
Her white blood cell count was 65,000/cmm3, haemoglobin was 6 gm% and platelet counts were 20,000/cmm3. Other routine blood investigations were normal. The combination of unilateral ptosis, monocular downgaze palsy and ipsilateral unreactive pupil suggested involvement of different structures innervated by the right oculomotor nerve. Only the LPS muscle, the pupillomotor fibres and the right IR (the primary depressor of the eye) were affected. The other muscles innervated by the right oculomotor nerve (IO, SR and MR) were spared. This constellation of signs was consistent with a partial oculomotor nerve involvement. The differential diagnosis was Holmes–Adie syndrome (as ptosis was very mild and initially missed, which was picked up on re-examination) or a lesion involving the oculomotor nerve in the subarachnoid space.
A magnetic resonance imaging scan of the brain was performed. It showed a 7.8 × 6 mm rounded T2-weighted and FLAIR hyperintensity with diffusion restriction in the right medial part of the midbrain (Figure 2). This was suggestive of a midbrain infarct involving the medial exiting fascicles of the oculomotor nerve and sparing the more lateral fascicles. As she had severe thrombocytopenia (20,000/cmm3), anti-platelets were contra-indicated. She complained of mild blurring of vision; however, this gradually improved within ten days. Two weeks later, she developed neutropenic sepsis, which required intensive treatment. She was subsequently transferred to palliative care and expired one month later.
The oculomotor nucleus is a multilevel complex midbrain nucleus which contains somatic motor and autonomic subnuclei. It contains bilateral subnuclei that innervate four ocular muscles (MR, IR, IO, SR) as well as two midline subnuclei that innervate the levator palpebrae superioris and pupils bilaterally (parasympathetic pupillomotor fibres from the Edinger Westphal nucleus).
As the fascicles exit the nuclear complex, they criss-cross and rearrange themselves into different configurations within the tegmentum of the midbrain, which are probably influenced by the relative positions of the subnuclei within the midbrain.1,2 The lateral to medial arrangement of fascicles is proposed to be in the following order: IO, SR, MR, LPS, IR and pupillary fascicles. The LPS and MR fascicles lie very close together and most reported cases have shown involvement of these two. In addition, some authors have proposed a rostro-caudal arrangement of these fascicles. The fascicles then exit the inter-peduncular fossa into the subarachnoid space.
The fascicles then undergo a further rearrangement in the subarachnoid space in preparation for their final fascicular arrangement. As the pupillary fascicles lie medial-most in the tegmentum, they lie supero-medially within the oculomotor nerve in the subarachnoid space. However, their final destination is the inferior division of the oculomotor nerve (Figure 2). Thus, by the time the oculomotor nerve enters the orbit through the superior orbital fissure, the pupillary fascicles will rotate inferiorly, and the final fascicular arrangement is evident. Usually, the oculomotor nerve divides into superior and inferior divisions within the orbit, although the division can occur more proximally at the fascicular level within the midbrain or the subarachnoid space, giving rise to a false-localizing divisional palsy.3 The superior division supplies the upper muscles (LPS and SR) and the inferior division supplies the rest (pupillomotor, IR, MR and IO muscles).
As the LPS, pupillomotor and IR fascicles lie at different poles of the oculomotor nerve, the only place where they are in close proximity to each other is within the crus cerebri.4 Elsewhere, throughout the course, these fascicles are widely separated. This fascicular peculiarity explains our patient’s partial oculomotor palsy due to infarction of the medial crus cerebri affecting the medial three fascicles in the medial midbrain (pupillary fibres, LPS and IR).
In conclusion, a midbrain infarct presenting with partial oculomotor palsy with unilateral mydriasis, ptosis and monocular downgaze palsy is uncommon. Such a combination should suggest a discrete lesion affecting the medial three oculomotor fascicles (pupillomotor, LPS and IR) in the crus cerebri of the midbrain.