A 17-year-old female presented to hospital with a four-day history of right upper quadrant pain and jaundice. She reported further non-specific symptoms of lethargy, nausea and dizziness. She had no past medical history of note.
Previous to admission she was on no regular medications and had used no over-the-counter medications including any herbal supplements. At the time of presentation, she reported no illicit drug use or any paracetamol ingestion. The patient further denied alcohol use or recent travel abroad.
There was no significant family history of liver disease. Her work as a horse groom further confirmed no exposure to other potential hepatotoxins. This includes industrial chemicals such as solvents for waxes or varnishes or any hepatotoxic fungi.
On admission her temperature was 36.4°C, pulse 82 bpm, blood pressure 110/65 mmHg, respiratory rate 16 and oxygen saturations 100%. Examination was positive for jaundice and right upper quadrant tenderness. There was no clubbing or palmar erythema. She had no spider naevi and there were no scratch marks of note. There were no other positive abdominal signs with no findings of distension, hepatomegaly or splenomegaly. Furthermore, there was no lymphadenopathy noted or any evidence of ascites. Urinalysis was also clear.
Laboratory findings showed evidence of hepatitis both biochemically and within her coagulation screen. The patient had a white blood cell count of 7.9 x 109/L (4.0-11.0) and a haemoglobin level of 139 g/L (115-165). A blood film was not performed. Serum electrolytes were normal with a serum creatinine of 57umol/L (53-78). Bilirubin was elevated at 231 umol/L (2-14), ALT was 2,054 u/L (8-22) and ALP 401 u/L (48-95). G-glutamyl transferase was 108 U/L (7-21). Paracetamol level was <3 mg/L and salicylate level <9 mg/L. The coagulation screen revealed a prothrombin time of 33.4 seconds (9.0-12.0) and an APTT of 50.7 seconds (20.0-30.0). The INR was 3.7.
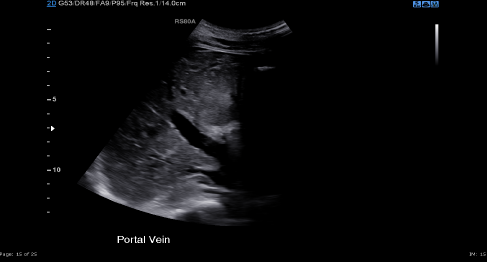
Abdominal ultrasonography revealed a patent portal vein with no reverse flow and no evidence of portal hypertension. The liver appeared normal. No gallstones were seen within the gallbladder with no evidence of any intrahepatic duct dilation being demonstrated (Figure 1). The spleen and both kidneys were reported as normal. A small quantity of free fluid was noted around the liver and a trace in the pelvis.
Figure 1 Patent portal vein
The patient proceeded to have a contrasted CT abdomen and pelvis scan. This reported a distended stomach and a slightly heterogeneous parenchymal density in the liver but normal gallbladder and biliary tract. No focal liver lesion was identified with a preserved portal vein and splenoportal architecture. The scan confirmed evidence of small volume peritoneal ascites (Figure 2).
Figure 2 Patent portal vein (arrow)
A urinary drug screen was negative. Anti-mitochondrial antibody, anti-smooth muscle antibody and anti-nuclear antibody were also negative. A CMV test was also negative, with serum IgG and IgM within normal range. Serum IgA was slightly elevated at 3.93 g/L. Tests for human immunodeficiency virus (HIV antigen/antibody test) were negative as were virology screens for Hepatitis A, B, C and E. These tests included Hepatitis A IgM, Hepatitis B Total Core Antibody, Hepatitis B surface, Hepatitis C antibody (anti-HCV) and Hepatitis E IgM and IgG. The patient also tested negative for syphilis total antibody.
With numerous negative findings, a test was requested for Epstein-Barr virus (EBV) antibodies, the result of which remained pending up to the point of liver transplantation. No IgM or PCR for EBV virus tests were requested.
Initially the patient was treated with N-acetylcysteine for a suspicion of possible paracetamol overdose. With a paracetamol level of <3mg/L and the patient denying any such history, this was deemed unlikely. The patient was then given three days of vitamin K 10mg, piperacillin with tazobactam and lactulose, as well as pabrinex and intravenous fluid. She was admitted to the Intensive Therapy Unit (ITU) for central access and increasing nursing requirements. Through her short stay on ITU the patient’s coagulation continued to deteriorate with a PT time of 52.8 seconds and an APTT as high as 92.8 seconds. The INR reached a peak of 5.1. This deteriorating coagulopathy was managed with a total of 6g fibrinogen and four units of FFP across two days.
During her ITU admission the patient became increasingly agitated and delirious. This was initially managed with quetiapine and haloperidol. The patient became increasingly encephalopathic and a decision was made to intubate. At this point the diagnosis remained unclear. Four days after her initial admission to ITU the patient was discussed with the regional liver unit and listed for liver transplantation. The patient received a successful whole sized graft from a donor.
The histological report of the explanted liver further raised the suspicion of a viral agent as a cause. The liver parenchyma showed widespread panacinar necrosis, moderately dense infiltrate of inflammatory cells and patchy hepatocyte ballooning with lobular disarray also present in these areas. There was severe patchy bilirubinostasis. Foci of confluent/bridging necrosis were present. Stains for iron, alpha 1 antitrypsin, HBsAg and copper were negative. Appearances were in keeping with a severe acute hepatitis with widespread multiacinar necrosis. The clinical circumstances were suggestive of a case of seronegative hepatitis and the report questioned a possible viral agent as the causative feature.
As the transplant was performed at a distant tertiary centre, imaging of the histology has not been made available.
Post-transplant a positive biochemical result was then returned for EBV Nuclear Antigen IgG.
Discussion
Acute liver failure (ALF) is a rare life-threatening disease that has a high mortality rate. Commonly seen in previously healthy adults, this multisystemic illness progresses after a significant injury to the liver, resulting in the progression of coagulopathy and encephalopathy within a short period of time.1,2 The mainstay of therapy of proven benefit remains emergency liver transplantation and despite advancements in intensive care management of ALF, mortality rates remain high.3
Although drug-induced liver injury and viral hepatitis are largely the most prevalent causes of ALF, no specific aetiology is found in a substantial proportion of cases reported.4 In up to 17% of cases the cause is indeterminate.5
The causes of acute liver failure are highlighted in Box 1.
Box 1 Causes of acute liver failure
- Herbal drugs and supplements
- Toxins such as industrial chemicals and solvents
- Paracetamol overdose
- Medications – NSAIDs, antibiotics and anticonvulsants etc.
- Autoimmune liver disease – autoimmune hepatitis
- Viral hepatitis
- Sepsis
- Metabolic disease – acute fatty liver of pregnancy, Wilson’s disease
- Budd-Chiari syndrome
- Malignancy
Frequently associated with infectious mononucleosis in adolescence or young adults, EBV, also known as human herpes virus,4 is a virus that commonly occurs only in humans. Laboratory testing can help distinguish between past or recent infection. The presence of IgM antibodies indicate recent primary infection with EBV, similarly positive PCR testing reflects a recent infection. The presence of IgG antibodies however, may reflect an infection sometime in the past. Nucleic acid antibodies to EBV develop usually 6-8 weeks after primary infection and can remain detectable for life.
In relation to ALF, primary EBV infection typically resolves without further clinical consequence. Although biochemical evidence of hepatocellular damage is common (within the acute phase of infection elevated transaminases are found in 80% of patients), hepatitis owing to primary EBV infection is usually mild and self-limiting.6,7
When we consider causes of ALF, EBV infection is an exceedingly rare cause, with primary EBV infection accounting for just 0.21% of adult ALF cases. Despite this, EBV-associated ALF has a very high case fatality rate.8
Though the medical literature reports very few cases of EBV-associated ALF, consideration of EBV virus as a potential cause remains of essential concern. Rapidly establishing a diagnosis of EBV-related ALF can assist with clinical management and potential use of antiviral agents.
Treatment of EBV-associated ALF with antiviral agents has only been rarely described in the literature, but determining such aetiology remains important for a number of reasons. Once the diagnosis is known, specific targeted therapies or antidotes may still be indicated. Moreover, determining the aetiology provides a plausible channel to predicting outcome.8
Conclusion
Though EBV-related ALF may be an under-recognised cause of ALF, our case highlights the importance of EBV serologies, and EBV DNA testing of serum and liver tissue. This may be of significant value in the evaluation of adult ALF patients with indeterminate ALF.
References
1 O’Grady JG. Acute liver failure. Postgrad Med J 2005; 81: 148-54.
2 Bernal W, Wendon J. Acute liver failure. N Engl J Med 2013; 369: 2525-34.
3 Lee W, Squires R, Nyberg S et al. Acute liver failure: summary of a workshop. Hepatology 2008; 47: 1401-15.
4 Tessier G, Villeneuve E, Villeneuve J. Etiology and outcome of acute liver failure: experience from a liver transplantation centre in Montreal. Can J Gastroenterol 2002; 16: 672-76.
5 Lee W. Etiologies of acute liver failure. Semin Liver Dis 2008; 28: 142-52.
6 Kofteridis D, Koulentaki M, Valachis A et al. Epstein Barr virus hepatitis. Eur J Intern Med 2011; 22: 73-76.
7 Kang M, Kim T, Shim K et al. Infectious mononucleosis hepatitis in young adults: two case reports. Korean J Intern Med 2009; 24: 381.
8 Mellinger J, Rossaro L, Naugler W et al. Epstein-Barr Virus (EBV) related acute liver failure: a case series from the US Acute Liver Failure Study Group. Dig Dis Sci 2014; 59: 1630-37.
